The Latest Pox On Our Houses
Monkeypox Brings The "Unknown Unknowns" Into The Foreground
“There are known knowns, things we know that we know; and there are known unknowns, things that we know we don't know. But there are also unknown unknowns, things we do not know we don't know.” — Donald Rumsfeld
Former Secretary of Defense Donald Rumsfeld’s analysis of the limitations of knowledge was much maligned at the time of its utterance (the Plain English Campaign would gift Rumsfeld their 2003 Foot in Mouth Award), and yet the quote lives on within the scientific research community, which has long recognized the concept of “unknown unknowns”.
Thus it becomes an ideal framework for assessing the media coverage of the current global monkeypox virus.
The Known Knowns: The Background On Monkeypox
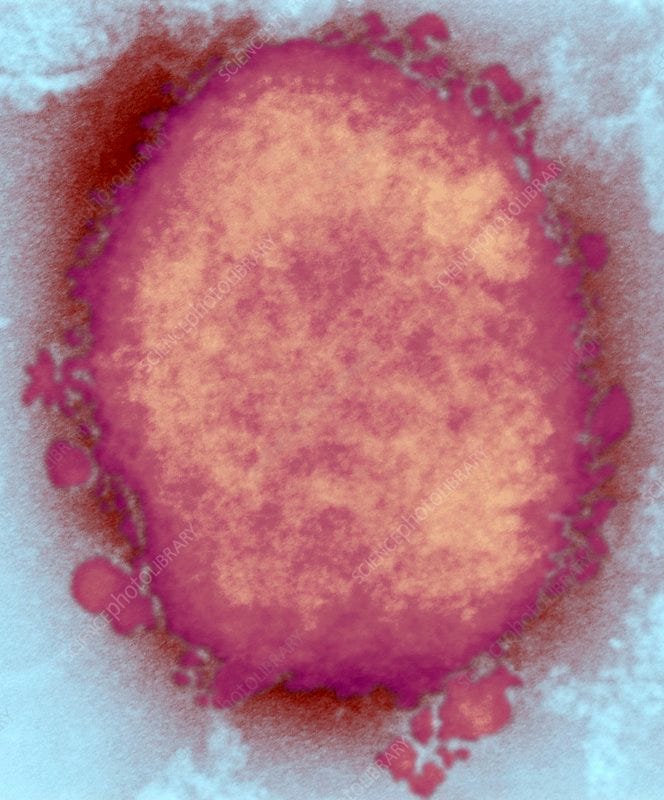
Monkeypox is a virus related to both the variola virus which causes smallpox and the vaccinia virus which is used as a vaccine against the variola virus.
Monkeypox is a rare disease that is caused by infection with monkeypox virus. Monkeypox virus belongs to the Orthopoxvirus genus in the family Poxviridae. The Orthopoxvirus genus also includes variola virus (which causes smallpox), vaccinia virus (used in the smallpox vaccine), and cowpox virus.
There are two distinct clades (variants) of the monkeypox virus—the Central African clade and the West African clade, with the Central African clade historically causing the more severe disease and resulting in the most deaths.
Monkeypox virus is an enveloped double-stranded DNA virus that belongs to the Orthopoxvirus genus of the Poxviridae family. There are two distinct genetic clades of the monkeypox virus – the Central African (Congo Basin) clade and the West African clade. The Congo Basin clade has historically caused more severe disease and was thought to be more transmissible. The geographical division between the two clades has so far been in Cameroon - the only country where both virus clades have been found.
Human-to-human transmission of the virus generally requires close contact with the respiratory excretions or skin lesions of an infected person. The close and prolonged contact requirement makes the virus considerably less transmissible than respiratory viruses such as SARS-CoV-2.
Human-to-human transmission can result from close contact with respiratory secretions, skin lesions of an infected person or recently contaminated objects. Transmission via droplet respiratory particles usually requires prolonged face-to-face contact, which puts health workers, household members and other close contacts of active cases at greater risk. However, the longest documented chain of transmission in a community has risen in recent years from six to nine successive person-to-person infections. This may reflect declining immunity in all communities due to cessation of smallpox vaccination. Transmission can also occur via the placenta from mother to fetus (which can lead to congenital monkeypox) or during close contact during and after birth. While close physical contact is a well-known risk factor for transmission, it is unclear at this time if monkeypox can be transmitted specifically through sexual transmission routes. Studies are needed to better understand this risk.
Beginning around 13 May 2022, cases of monkeypox infection have been reported to the WHO from countries outside the region in Africa where the disease is known to be endemic, and with no established travel links to that region. As of 21 May, all confirmed cases of monkeypox within this current outbreak have been identified as belonging to the less severe West African clade, which has a mortality rate of around 1% (the Central African clade has a mortality rate of 10%).
Side note: media reports which reference a 10% mortality rate are referencing the Central African clade, not the West African clade,which is the one currently in global circulation. This subtle factual error is the result of considerable media exaggeration of the severity of the outbreak.
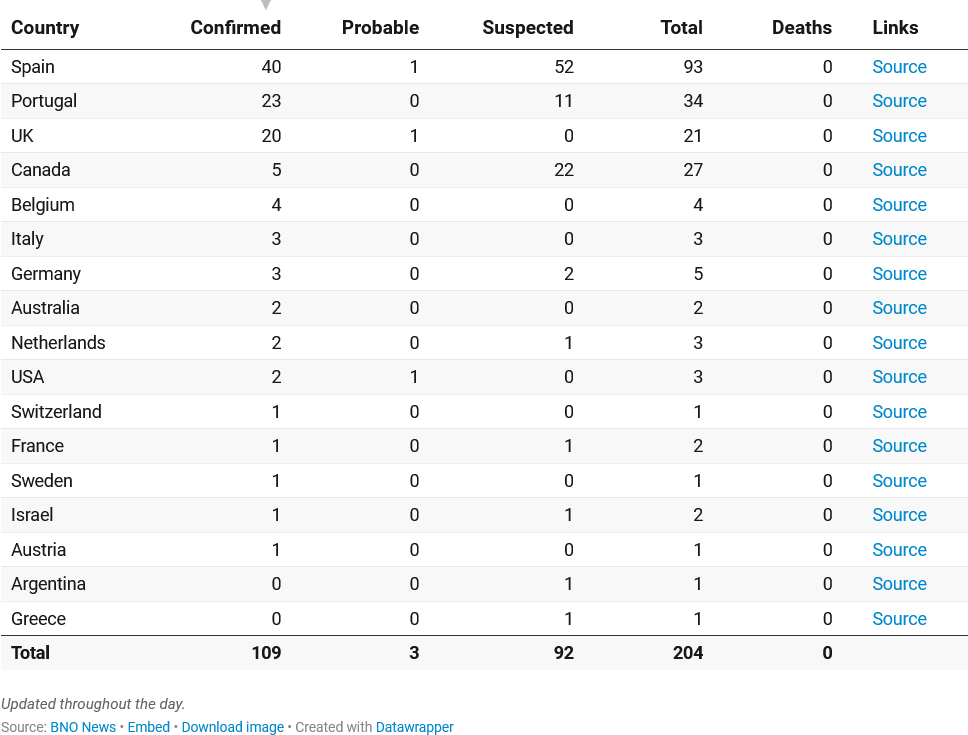
As of this writing, there are 109 confirmed cases of monkeypox, 3 probable cases, and 92 suspected cases. As the outbreak is ongoing, these numbers will change substantially day by day.
One apparent nexus for community spread in the current outbreak appears to be the Darklands Festival in Antwerp, Belgium, a homosexual fetish festival intended to create “a unique spectacle of fetish brotherhood”.
The Darklands Festival in Antwerp has been linked to all three confirmed cases of the disease in Belgium following four days of partying that began on May 5, according to AFP. The festival’s organizers said on their website that the Belgian government had asked them to inform attendees that the outbreak was likely caused by a festival-goer bringing the sickness from abroad.
While monkeypox is not considered a sexually transmitted disease, one apparent common denominator among the cases reported thus far is that they are mainly occurring among men who acknowledge having sexual contact with other men.
In several countries, many confirmed cases have been in young men who had sex with other men. Although sexual contact may play a role, monkeypox isn’t a sexually transmitted disease. A few cases were caused by exposure to a household member with monkeypox, and officials are still investigating how each infected person contracted the virus, Dr. Elsayed said.
Broadly speaking, these are the “known knowns” about the global monkeypox outbreak.
The Known Unknowns: Specific Treatments For Monkeypox
At this time, there are no known proven treatments specifically for monkeypox. Instead, treatment involves antivirals and countermeasures designed specifically for smallpox. Vaccination for monkeypox is done using smallpox vaccines.
Currently, there are no proven treatments specifically for monkeypox. Instead, cases of monkeypox can be treated with medical countermeasures designed for the closely related smallpox virus. There are currently 3 smallpox vaccines that could be used in the US, 2 of which are licensed for smallpox and the other could be used for smallpox under an investigational new drug (IND) protocol. The two licensed vaccines for smallpox are JYNNEOS™ (also known as Imvamune or Imvanex) and ACAM2000®, of which JYNNEOS™ is also licensed for monkeypox.
The US Government has recently purchased an additional 13 million doses of the JYNNEOS™ vaccine, ostensibly in preparation for a larger monkeypox outbreak here in the US. JYNNEOS™ is considered to be roughly 85% effective in preventing monkeypox, based on data from Africa.
The lack of monkeypox-specific antivirals is proving a boon for smallpox antiviral manufacturers. Biotech companies such as Emergent Biosolutions and SIGA Technologies, which produce smallpox antivirals, are seeing their share prices rise significantly.
SIGA produces the antiviral tecovirimat, which is sold in the US as TPOXX, while Emergent produces the ACAM2000 smallpox vaccine and recently struck a deal with another drug company, Chimerix, to acquire exclusive rights to their smallpox antivirual Tembexa, which is FDA approved.
The Unknown Unknowns: What Is Really Happening?
Coming in the aftermath of the COVID-19 Pandemic Panic, the spread of monkeypox across regions where the pathogen is not known to be endemic makes the disease natural fodder for speculations of all kinds.
As Igor Chudov has documented, there was the unusual “monkeypox preparedness exercise” in the spring of 2021, which posited a start date for the outbreak of May 15, only a few days off from the actual date cases first began being reported to WHO.
Given the relative rarity of monkeypox outbreaks and the extreme rarity of the disease spreading beyond the African countries where it is endemic, why health experts even felt the need to prepare for such an outbreak is itself a question. That this exercise took place barely a year before an actual global outbreak of monkeypox is the most amazing of coincidences.
It should also be noted that the lack of specific antiviral treatments and vaccines for monkeypox is itself remarkable. As I learned while digging into the background of US biological “threat reduction” programs, there was an international effort in 2002 to study the monkeypox genome, led by Russia’s premier biolab (and formerly the Soviet Union’s premier bioweapons facility), State Research Center of Virology and Biotechnology VECTOR.
Yet the efforts of Nunn-Lugar “threat reduction” programs have not been touted as proof of the virtues of such forward-thinking preparedness by media coverage of the monkeypox outbreak. Moreover, despite the monkeypox genome having been mapped some 20 years ago, researchers are still calling for “better understanding” of the virus’ genomic evolution and structure.
The experts further agreed on the need for a better understanding of the genomic evolution and changing epidemiology of orthopox viruses, the usefulness of in-field genomic diagnostics, and the best disease control strategies, including the possibility of vaccination with new generation non-replicating smallpox vaccines and treatment with recently developed antivirals.
Biological “threat reduction” for a variety of infectious pathogens, including monkeypox, has been a mainstay of Nunn-Lugar-related funding in the past, yet, curiously, none of the amassed body of information seems to be coming to the fore now. The mapping of the monkeypox genome, which was written up in the peer-reviewed journal Virology in June of 2002, has not been referenced in media articles on the monkeypox outbreak that I have read; with such study already having been done, monkeypox should be far less mysterious than it is presented as being in the media.
Another speculation that as yet has not been raised in the media is whether or not this global outbreak indicates the emergence of reservoir hosts for the virus outside of central and western Africa. An expansion of the endemic region for monkeypox arguably presents a greater risk going forward than the current cases.
Perhaps the most significant unasked question in the corporate media is whether or not the strain of monkeypox currently showing up around the globe shows any indication of being weaponized.
The NTI tabletop exercise which Igor discusses involved an unusual and potentially weaponized form of the virus.
Developed in consultation with technical and policy experts, the exercise scenario portrayed a deadly, global pandemic involving an unusual strain of monkeypox virus that first emerges in the fictional country of Brinia and eventually spreads globally. Later in the exercise, the scenario reveals that the initial outbreak was caused by a terrorist attack using a pathogen engineered in a laboratory with inadequate biosafety and biosecurity provisions and weak oversight. The exercise scenario concludes with more than three billion cases and 270 million fatalities globally. As part of the scenario development process, NTI conducted a virtual consultation with experts in December 2020. (See Appendix A for the list of participating experts.)
With the total number of cases in this current outbreak around two hundred, the reality of the outbreak seems fairly far from the hypothesized scenario from last year. Yet the contemplation of monkeypox as a bioweapon also leads us back to the reality that the institutions which have studied the full monkeypox genome have in the past been involved in formal bioweapons research and development.
Is this a weaponized strain of monkeypox, or a “vaccine challenge” strain intended to test monkeypox vaccines? What has been reported thus far does not present any evidence that it is, but, given the past examples of Nunn-Lugar “threat reduction” becoming “threat creation”, we owe it to ourselves to least acknowledge the possibility.
So far, no one has died in this current outbreak of monkeypox. Yet even so, the greatest potential dangers lie in all the things we as yet do not know, and in all the questions we do not know enough to ask.
Monkeypox is but the latest reminder of the importance in research of the “unknown unknowns”.



Fun fact: Rumsfeld was a Pharm guy.
Quote of 2022..."A pox on all their houses."....W.H.O, WEF, Bill Gates, Klaus Schwab, Turdeau, Biden, vaccine manufacturers, MSM, (fill in the blank)......